Benign Gastro Oesophageal Disorders
This is an overview of Benign Gastro-Oesophageal Disorders such as Gastro-Oesophageal Reflux Disease (GORD), Hiatus Hernia, Barrett’s Oesophagus and Achalasia.If you have been diagnosed with one of the Benign Gastro-Oesophageal Disorders, your surgeon will help you understand your condition, and the surgery that you may require. We discuss the causes and symptoms, the types of applicable surgery at The Surgeons Collective in Perth, as well as dietary recommendations as part of the typical aftercare program for these treatments. Our specialist surgeons in Perth build on years of experience performing surgeries for these disorders, with excellent clinical outcomes.
Gastro-Oesophageal Reflux Disease (GORD)
What is reflux disease?
GORD occurs when the stomach content flows back upwards into the oesophagus (also called the gullet or food pipe) causing irritation and inflammation to its inner lining (mucosa) . This leads to symptoms most patients describe as:
- a burning sensation (heartburn) in the upper abdomen, radiating to the breast bone (and sometimes experienced as chest pain)
- regurgitation of gastric juices
- excessive belching
- stomach fluid content flowing all the way to the throat or aspirating down into lungs causing chronic coughing, wheezing or sore throat, as “atypical” symptoms in more severe cases.
At The Surgeons Collective, our team of top surgeons and medical staff are totally committed to delivering excellent outcomes, when we work out your personalised care plan for Benign Oesophageal Disorders. Throughout your treatment, our whole team will be by your side to support you and to provide an excellent care experience.
Gastro-oesophageal reflux disease
Learn more about reflux disease.
What causes GORD?
When is surgery needed?
What diet applies?
Hiatus hernia
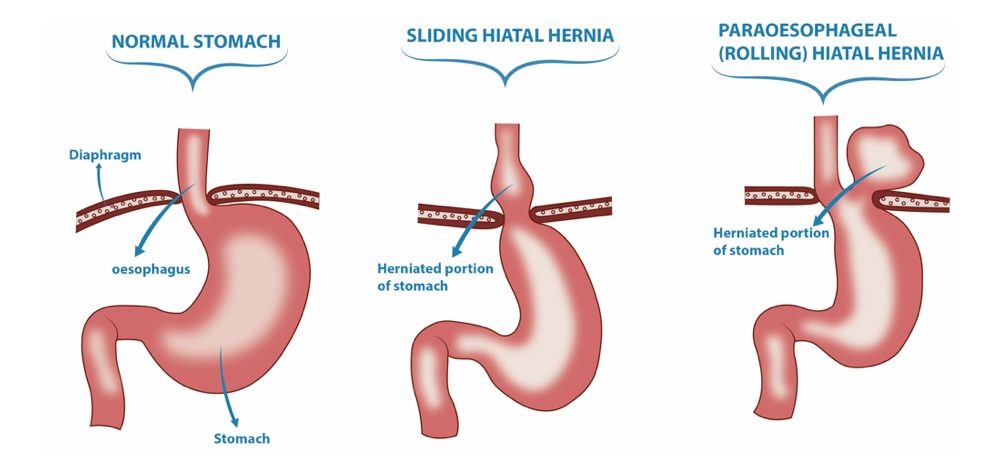
The oesophagus or “food pipe” is a muscular tube that begins in your upper neck. The pipe passes downwards into your chest and then crosses your abdomen. This happens through an “opening” (hiatus) within a dome shaped muscle structure, which separates the chest and abdomen. The muscle structure is known as the diaphragm.
Once the oesophagus crosses this opening, it then empties the food that we eat into the stomach, which sits right below the diaphragm. A “hiatal hernia” is a condition where the muscles of the hiatus have become weakened and become “stretched”. As a result, the opening (or hiatus) grows larger, and organs such as the stomach, spleen, or intestines, can now slip upwards into the chest.
What are the symptoms of hiatus hernia?
Benign oesophageal disorders such as a hiatus hernia will not necessarily result in clear symptoms, and some patients are asymptomatic. But with a larger hiatal hernia, the disorder can cause reflux or heartburn, difficulty in swallowing or chest pains. In serious cases, the hiatal hernia is large enough that the entire stomach could slip in the chest and cause a “twisting” (gastric volvulus). This is very uncommon condition but it requires an emergency surgery to untwist the stomach and to return it into the abdomen.
About Us
At The Surgeons Collective we work as a team of expert surgeons, as well as hepatologists, gastro-enterologists and accredited dietitians.
How is hiatus hernia diagnosed?
At The Surgeons Collective, your team of specialist surgeons will help you get a clear diagnosis. It’s important to go to a specialist clinic to obtain clarity about the surgical options that are available to treat a hiatus hernia. It could be diagnosed with a combination of X-ray or CT scan imaging and endoscopy. Depending on your situation, our surgeons can also organise a barium swallow X-ray to gather information, to help plan for potential surgery. We know that going through this phase of uncertainty and waiting for test results can be stressful. At any stage, we will commit to providing excellent care, so you feel comfortable and well informed about your treatment journey. Our team of doctors, surgeons and health professionals firmly commit to your comfort before, during and after your treatment or surgical intervention.
How is hiatus hernia treated?
Hiatus hernia surgery is most commonly performed via laparoscopic surgery and it involves:
- Returning the slipped stomach back to its normal location in the upper abdomen.
- Repairing the hiatal hernia using non-absorbable surgical sutures. Sometimes, a “mesh” is used in certain circumstances to help strengthen the repair and reduce risk of recurrence of the hernia.
- “Fundoplication” - using the upper portion of the stomach (known as the fundus) to form a “wrap” around the lower oesophagus to re-create a one-way “valve” to help reduce reflux after your surgery.
Barrett’s oesophagus
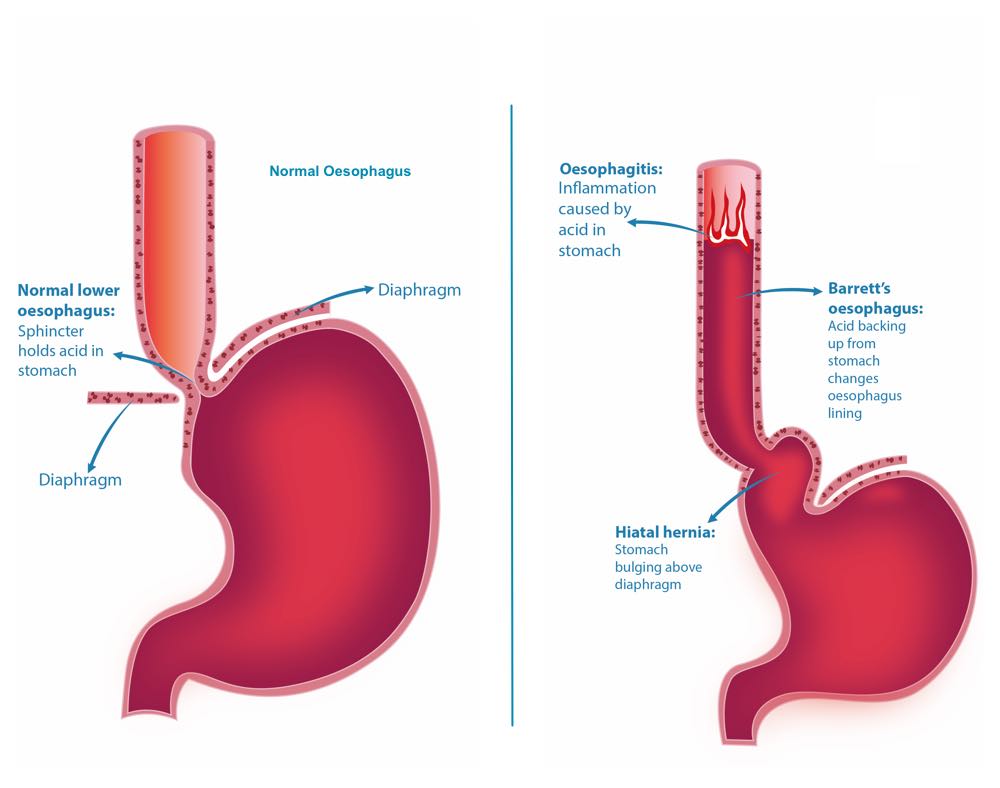
What is barrett's oesophagus?
Another type of benign oesophageal disorders is Barrett’s oesophagus. This condition is highly associated with long standing reflux disease. It is diagnosed with an endoscopy and is characterised by abnormal transformation of the inner lining of the oesophagus. That transformation is a result of acid reflux, and the injury it causes on the lining. The reason why it is important to go to a specialist clinic for this condition is that the abnormal cells could be “pre-cancerous” (dysplasia). Our team of highly specialised surgeons in Perth always commit to providing an excellent care experience, including a reliable and detailed diagnosis. This allows our team to plan the most suitable treatment, so the progression of adenocarcinoma (a form of cancer in the oesophagus) can be avoided.
How is it treated?
This will depend on several factors but it depends on the severity of your condition, and on the presence of pre-cancerous cells. Treatment may involve comprehensive endoscopic surveillance to identify pre-cancerous abnormal cells early on. Your personalised care plan may involve anti-acid medications such as proton-pump inhibitors, or endoscopic ablative therapy. If pre-cancerous or early cancer is identified, then some patients may be considered for a major resectional surgery. Whatever the diagnosis, our team of expert surgeons will use their extensive experience in this field to deliver the best possible surgical outcomes.
Achalasia
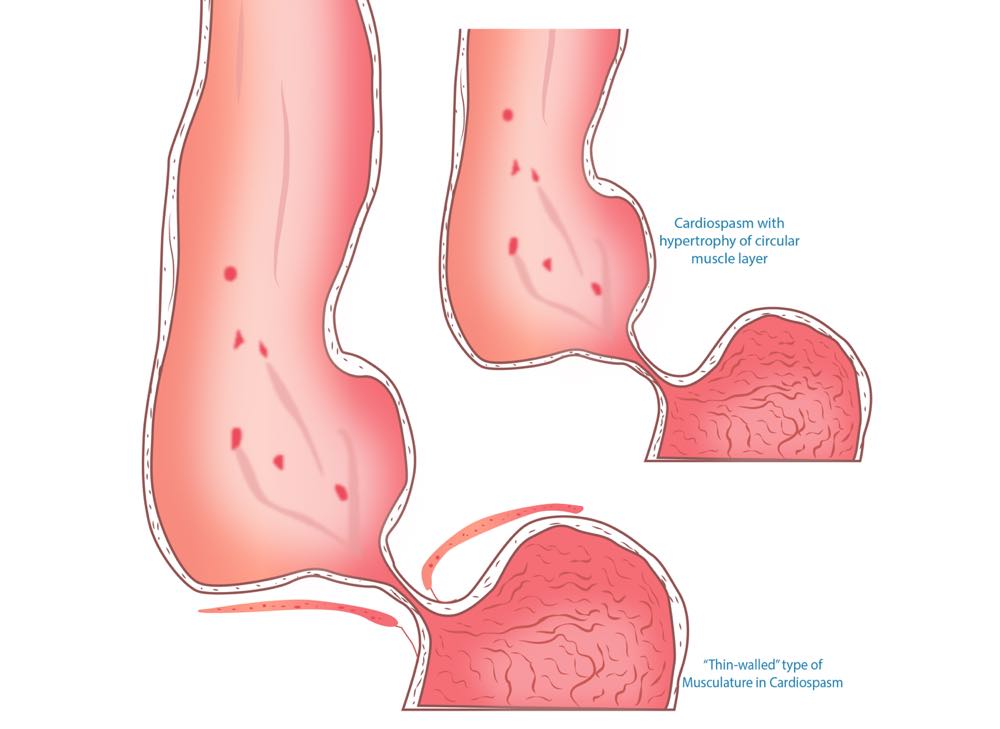
What is achalasia?
This is a very rare condition which is characterised by abnormality in the function of the muscles in the lower oesophagus (food pipe) known as the “lower oesophageal sphincter” (LES). The LES acts as a specialised valve for food to pass down through the oesophagus into the stomach. It also prevents contents from flowing back up, what we call reflux. In achalasia, the LES is unable to relax or open in a normal response to the swallowing of food. The food becomes “stuck” in the lower oesophagus.
As a result, you would find it hard to swallow, and the symptom may get worse over time. If left untreated, patients may become unable to eat adequately, lose weight and become malnourished. Until today, the underlying cause of Achalasia is not fully understood.
How is it diagnosed?
Patients with achalasia initially will experienced symptoms similar to GORD. Sometimes the treatment that is prescribed will be similar to a treatment for GORD, with anti-acid medications. If the condition isn’t managed with medication, your specialist surgeon may recommend an upper GI endoscopy, or further tests such as an oesophageal manometry to confirm the diagnosis.
How is it treated?
Treatment for achalasia will vary from patient to patient and will need to be reviewed carefully by your treating surgeon at The Surgeons Collective. Options could involve medications, endoscopic treatment or surgery. In most cases, the gold standard operation would involve a myotomy, whereby the abnormally “shut” LES muscle is incised surgically, so food can pass through. The procedure is most often performed laparoscopically.
At any point in time, our team of highly experienced surgeons will work together to make sure you receive the best possible, personalised care plan. Your comfort as a patient, kindness as you go through this journey, and a relationship of trust with your surgeon, are essential in our role as your specialist surgical centre.
What diet applies for benign oesophageal disorders?
Achalasia - With difficulties swallowing, you may need a personalised diet to improve your nutritional intake, as normal foods and liquids can get stuck, cause reflux or regurgitation. Our focus as a team of dietitians will be to prevent further weight loss, and to adjust the texture of you diet.
Barrett’s oesophagus - If your condition is linked to being overweight, our dietitians will help you make lifestyle changes to facilitate a healthy diet. Other lifestyle changes can include letting go of your smoking habits, not eating 2 hours before going to bed and eating smaller portions in general. If you undergo surgery (Nissen Fundoplication), you will require a puree diet for 4 weeks after your surgery and your dietitian here at The Surgeons Collective in Perth will help ensure that your nutritional intake is adequate.
Hiatus hernia - Hiatus Hernia can be associated with being overweight and weight loss may be indicated to help reduce your symptoms. Your Surgeons Collective dietitian will assist you with making important changes to your diet and facilitate weight loss.
Reflux - Making dietary changes may help to manage your reflux. Reflux is often associated with being overweight or obese. Typical dietary changes that may help include avoiding carbonated beverages, avoiding alcohol, and limiting spicy, acidic, fatty foods, caffeine and chocolate. It may also help to have smaller frequent meals and not to eat within 2 hours of going to bed.
Why The Surgeons Collective in Perth?
If you have been diagnosed with any of the Benign Oesophageal Disorders, it’s essential to speak to our specialists at The Surgeons Collective to get the most suitable treatment. Why come to us?
- We are a team of experienced Perth surgeons, who have been performing a wide range of surgery types for many years. Because we use the latest laparoscopic and minimally invasive technology, we are able to deliver excellent surgical outcomes with minimal discomfort.
- As a team of professionals, we commit to a personalised and a caring patient experience. Not only as you obtain a detailed diagnosis, but also in the days before your surgery and during your aftercare program. At The Surgeons Collective in Perth, we believe in the importance of kindness, trust and patient comfort as you go through your treatment journey.
- We also go out of our way to reduce your wait times to see our surgeons. Then we commit to ensuring that your care plan is organised in the timeliest manner. Always adapted to your personal needs. Please call The Surgeons Collective in Perth on (08) 6163 2800 if you would like to make an enquiry, we will be happy to assist you.
Contact us
THE SURGEONS COLLECTIVE
McCourt St Medical Centre
Level 1, Suite 10, 2 McCourt Street
West Leederville,
Perth 6007, WA
THE SURGEONS COLLECTIVE
Monday - Thursday | 8:30am - 4:30pm
Friday | 9:00am - 1:30pm
